Применение мультимодальной радиочастотной технологии для коррекции возрастных изменений нижней трети лица и шеи
Erez Dayan, MD
Paolo Rovatti, MD
Sherell Aston, MD
Christopher T. Chia, MD
Rod Rohrich, MD
Spero Theodorou, MD
Background: Nonexcisional facial skin tightening has long been an elusive goal in aesthetic surgery. The “treatment gap” includes cases who are not “severe” enough for excisions surgery but not “mild” enough for most traditional noninvasive aes thetic modalities. In this retrospective review, we present the largest evaluation to date of radiofrequency (RF) skin tightening technology combination including bipolar RF (FaceTite; InMode) and fractional bipolar RF (Fractora modified to Morpheus8; InMode).
Methods: A multicenter retrospective study was conducted between January 2013 and December 2018 using a combination of bipolar RF and fractional bipolar RF for the treatment of facial aging. Data collection included demographic informa tion, Baker Face/Neck Classification, amount of energy used, adverse events, and patient satisfaction. Four cadaver dissections were also conducted to correlate the underlying neuromuscular anatomy with RF treatment of the lower face and neck. Results: Two hundred forty-seven patients (234 women and 13 men) were included in the study. Average age was 55.1 years (SD, ±8), body mass index was 24.3 (±2.4), and 9% (23/247) of patients were active smokers at the time of treatment. Patients had an average Baker Face/Neck Classification score of 3.1 (SD, ±1.4). The procedure was performed under local anesthesia in 240/247 cases (97.2%). Patients objectively improved their Baker Face/Neck Classification score by 1.4 points (SD, ±1.1). Ninety three percent of patients indicated that they were pleased with their results and would undergo the procedure again. Complications recorded for our cohort included pro longed swelling >6 weeks (4.8%, 12/247), hardened area >12 weeks (3.2%, 8/247), and marginal mandibular neuropraxia (1.2%, 3/247), which all resolved without further intervention. When considering possible control variables, age seems to be a significant factor. That is, older patients were more likely to benefit from a larger magnitude of the treatment effect (as demonstrated by a decrease in the Baker rating from pre- to posttreatment) when compared with younger patients. However, both groups did demonstrate significant improvements across time.
Conclusion: While this combination RF treatment (FaceTite bipolar RF and fractional bipolar RF) does not aim to replace a facelift/necklift in appropriate candidates, it does broaden the plastic surgeons’ armamentarium to potentially fill a treatment gap. (Plast Reconstr Surg Glob Open 2020;8:e2862; doi: 10.1097/ GOX.0000000000002862; Published online 26 August 2020.)
From *Plastic and Reconstructive Surgery, Avance Plastic Surgery
Institute, Reno/Tahoe, Nev.; †Studio Dott. Rovatti, Verona, Italy;
Plastic and Reconstructive Surgery, Manhattan Eye, Ear & Throat Hospital, New York, N.Y.; §Plastic and Reconstructive Surgery, BodySculpt, New York, N.Y.; and Plastic and Reconstructive Surgery, Dallas Plastic Surgery Institute, Dallas, Tex.
Received for publication November 4, 2019; accepted March 25, 2020.
Copyright © 2020 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of The American Society of Plastic Surgeons. This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-No Derivatives License 4.0 (CCBY-NC-ND), where it is permissible to download and share the work provided it is properly cited. The work cannot be changed in any way or used commercially without permission from the journal.
DOI: 10.1097/GOX.0000000000002862
Disclosure: Dr. Dayan is consultant at InMode; he receives book royalties from Thieme & Elsevier and is a co-investigator of Allergan, Galderma, and MTF. Dr. Rovatti is consultant at InMode. Dr. Aston is consultant at InMode. Dr. Chia is consultant at InMode. Dr. Rohrich receives book royalties from Thieme and instrument roy alties from Micrins. He is a co-investigator of Allergan, Galderma, MTF, and InMode. Dr. Theodorou is consul tant at InMode.
Related Digital Media are available in the full-text version of the article on www.PRSGlobalOpen.com.
INTRODUCTION
Nonexcisional correction of facial soft tissue lax ity has long been an elusive goal in aesthetic surgery. Improvements in skin texture, dyschromias, and defla tion are achievable with chemical peels, lasers, micronee dling, and fillers. Areas of neck adiposity may be treated using liposuction, deoxycholic acid (Kybella; Allergan, Dublin, Ireland), and cryolipolysis (CoolSculpting; Allergan), with limited improvements in properly selected patients. However, even in cases where these treatments appear successful, skin and soft tissue laxity often remain uncorrected.
There are 3 groups of patients with facial skin laxity that we characterize as part of a “treatment gap”: (1) young patients whose skin redundancy is not “severe” enough to justify a traditional excision procedure (ie, facelift/neck lift), but also not “mild” enough to treat with liposuction or noninvasive procedures alone; (2) patients who have already undergone a facelift or necklift, who present with recurrent laxity, and (3) patients who may benefit from traditional face/necklift but want to avoid surgery and are willing to accept a more modest improvement.
Energy-assisted skin tightening procedures have rapidly evolved over the past decade. Multiple technologies includ ing laser, high-intensity focused ultrasound, and radiofre quency (RF) have been developed in an attempt to meet this rising demand.1–8 RF technology has steadily gained popularity since the early 2000s, with consecutive increases annually of 10% or more.9,10 These gains encompass aes thetic surgery and numerous nonaesthetic applications (tissue electrodissection, cardiac catheter ablation, oph thalmic surgery, etc).7 Through impedance of electromag netic current, RF waves lead to differential heating across distinct tissue types, consistent with Ohm’s law (energy = current2 × impedance × time). For example, adipose tis sue is less conductive than water (higher impedance) and leads to generation of temperatures higher than those generated by muscles. Once soft tissue temperatures reach 50°C and those of the skin surface reach 40°C–42°C, there is a trigger to induce neocollagenesis, angiogenesis, and elastogenesis. Through different applications of RF energy (ie, monopolar, bipolar, multipolar, microneedling), sub dermal adipose remodeling and long-term soft tissue con traction can be safely and consistently achieved.
An increasingly popular soft tissue tightening tech nique of the lower face and neck has been a combi nation procedure (Embrace Protocol; InMode, Lake Forest, Calif.) using bipolar RF (FaceTite; InMode) and fractional bipolar RF (Fractora modified to Morpheus8; InMode Aesthetics, Lake Forest, Calif.).11 The purpose of this study was to evaluate this combination therapy in the largest study to date.
METHODS
A multicenter retrospective study was conducted eval uating treatments from January 2013 to December 2018 (New York, N.Y.; Dallas, Tex.; and Verona, Italy) using a combination of bipolar RF (FaceTite; InMode Aesthetics) and RF microneedling (Fractora modified to Morpheus8;
InMode Aesthetics) for the treatment of facial aging. Procedures were performed by all the authors of this study (E.D., S.T., P.R., R.J.R., C.T.C, S.A.).
All the patients voluntarily presented to respective plastic surgery practices with a desire to improve facial aes thetics. Patients included in the study were deemed to fit into 1 of the 3 aforementioned treatment gaps. Exclusion criteria included active infection, collagen disorders, immunocompromised state, medications that mitigate inflammatory response, and propensity for keloids/hyper trophic scaring. Valcyclovir was given to patients with a his tory of herpes simplex. All Fitzpatrick types were included in this study.
Patients were all marked in a standardized manner, identifying first the mandibular border and jowls bilat erally. The jowls were subdivided into zone 1 (above the mandibular border) and zone 2 (below the mandibular border). Areas of localized adiposity in the lower face and neck region were marked. Nontreatment zones were iden tified by carrying a line inferiorly perpendicular to the lip commissures (ie, marionette lines). The area medial to these lines was avoided to preserve marginal mandibu lar innervation to the depressor anguli oris, mentalis, and depressor labii inferioris. Five access points were identi fied: (1) the submental midline, (2) 1–2cm inferior to the mandibular parasymphysial/body junction, (3) postauric ular (two of the access points were bilateral). (See Video 1 [online], which displays bipolar RF markings.)
Depending on clinical circumstances and patient desires, cases were performed either under general or under local anesthesia. In cases of local anesthesia, patients were premedicated with oxycodone (5mg) and benzodiazepam (5mg) or both. Access sites were each injected with 2–4ml of 2% lidocaine with epinephrine. A 14-gauge needle was used to make access ports that were slightly dilated with Stevens scissors. A spinal needle was used to slowly infiltrate tumescent solution (1g lidocaine per liter of lactate Ringer’s solution) from deep to superfi cial, starting in the pre-platysmal plane and moving to the subdermal plane (approximately 100–150ml of tumescent total). At the conclusion of tumescent infiltration, the can nula was passed through the subdermal plane to confirm adequate analgesia.
In all cases, bipolar RF was performed first. The RF settings included an internal temperature cutoff of 68°C and external cutoff temperature of 38°C. The RF cannula was used to pretunnel treatment areas for ease of treat ment. The predetermined treatment areas were systemati cally heated to avoid heat loss when treating wide areas. RF application was performed on retrograde movement of the cannula and stopped within 1cm of the access port to prevent overheating this area. Audible and visual cues from the RF console were used to assess temperature of tissues, and treatment was stopped after 1 minute of reach ing target internal and external temperatures. (See Video 2 [online], which displays the bipolar RF technique.) Fractional bipoar RF (Fractora modified to Morpheus8; InMode Aesthetics) was subsequently used at a depth of 2mm and energy of 30 with 50% overlap. The handpiece was applied firmly and perpendicular to the treatment area before delivery of RF energy pulses. (See Video 3 [online], which displays fractional RF technique.) In patients with thinner skin or darker Fitzpatrick types, energy settings were reduced by 20%. Patients were seen at 1-week and at 1, 3, and 6-month intervals.
Data evaluated included demographic information, prior procedural history, anesthesia, medications, Baker Face/Neck Classification, amount of energy used, and adverse events. The primary outcome evaluated was pre and post-procedure Baker Face/Neck Classification. Three independent plastic surgeons graded the pre- and postprocedure photographs, and subsequently a t test was used to determine statistical significance. Repeated mea sured analysis of variance test was used to determine any impact of control variables.
Additionally, 4 cadaver dissections were conducted to correlate the underlying neurovascular anatomy to access points and application of RF energy. These cadaver specimens were treated with the combination procedure mentioned previously, and dissections were subsequently performed to identify proximity and the potential impact on underlying specific neurovascular structures (ie, mar ginal mandibular nerve, facial vessels, etc).
RESULTS
Two hundred forty-seven patients (234 women and 13 men) were included in the study. Average age was 55.1 years (SD, ±8), body mass index was 24.3 (±2.4), 9% (23/247) of patients were active smokers at the time of treatment, 2% (5/247) of patients had prior neck liposuction, and 8.5% (21/247) of patients had prior facelift/necklift. Patients had an average Baker Face/Neck Classification score of 3.1 (SD, ±1.4). The procedure was performed under local anesthesia in 240/247 cases (97.2%) (50ml 2% lidocaine, 1.5mg epinephrine, 1.5ml bicarbonate, in 1L or lactated Ringer’s solution), and 2.8% (7/247) of patients underwent the procedure under general anesthe sia or intravenous sedation. Average procedure time was 58 minutes (SD, ±23). All patients were given Valium and cephalosporin antibiotics before the procedure.
Average energy used per jowl was 3.2 kJ (SD, 1.1). Patients objectively improved their Baker Face/Neck Classification score by 1.4 points (SD, ±1.1). Ninety-three percent of the patients indicated they were pleased with their results and would undergo the procedure again. Average follow-up time was 2.1 years (SD, ±1.1).
To test the efficacy of the treatment, a 1-way, repeated measure t test was conducted. A decrease in the mean val ues of pretest to posttest Baker Face/Neck Classification rating would indicate a positive effect of the treatment. Indeed, the t test demonstrated a favorable effect of the treatment in all the 247 patients. The pretest mean value was 2.66 (SD = 0.72), and the posttest mean value was 1.86 (SD = 0.64). This mean difference (μ = 0.81, SD = 0.46) was statistically significant: t(237) = 27.34, P < 0.001, and the effect size was large (D = 1.76). In other words, the mean values of the patients’ Baker Face/Neck Classification decreased as a result of the treatment. (See supplemental figure 1, Supplemental Digital Content 1, which displays pre- and posttreatment Baker Face/Neck Classification scores, http://links.lww.com/PRSGO/B410.) However, it is also possible that several control variables may have had an unhypothesized effect on the relation ship. Thus, a 1-way, repeated measures analysis of variance test was conducted, inclusive of control variables. These control variables were (1) gender, (2) smoking habit, (3) liposuction history, (4) weight, (5) age (dichotomized at the median value, 55), (6) body mass index, (7) right jowl energy (in kJ), (8) left jowl energy (in kJ), and (9) neck energy (in kJ). Although 247 valid cases were pres ent, complete data were available for only 238 patients; thus, data from 9 patients were excluded in these analyses. The following table presents the mean values or percent ages of the control variables in the overall fitted model. (See table, Supplemental Digital Content 2, which displays the descriptive statistics, http://links.lww.com/PRSGO/B411.)
When considering the overall model, it is clear from the analysis that the treatment was effective in reducing the Baker Face/Neck Classification rating: pretreatment Baker classification μ = 2.62 (SE = 0.03), pretreatment Baker classification μ = 1.84 (SE = 0.03); F(1, 208) = 11.36, P = 0.001. None of the control variables was statistically significant, except for age. A significant treatment by age interaction effect was present: F(1, 208) = 17.53, P < 0.001. This simply indicates that the Baker Face/Neck Classification pre- and posttreatment ratings are different at different age groups. The mean values demonstrates that while older patients seem to benefit from the treat ment more than younger patients by a larger magni tude, both age groups still show marked and significant improvements in their Baker Face/Neck Classification scores from pretreatment to posttreatment, as evidenced by Supplemental Digital Content 3. (See supplemental figure 2, Supplemental Digital Content 3, which displays Baker Face/Neck Classification scores by treatment age, http://links.lww.com/PRSGO/B412.)
Complications recorded for our cohort included pro longed swelling >6 weeks (4.8%, 12/247), hardened area >12 weeks (3.2%, 8/247), and marginal mandibular neu ropraxia (1.2% 3/247), which all resolved without further intervention. There were no repeat treatments or cases requiring operative interventions following RF treatment.
DISCUSSION
While this combination RF treatment (FaceTite bipo lar RF and fractional bipolar RF) does not aim to replace a facelift/necklift in appropriate candidates, it does broaden the plastic surgeons’ armamentarium to poten tially fill a treatment gap. Also, it provides patients with an option to improve facial soft tissue laxity without a tradi tional surgery.
In recent years, RF has emerged as an effective treat ment to achieve nonablative skin tightening.6,7,10,12,13 Heating the dermal tissue to 42°C has been shown to trig ger a healing cascade that leads to stimulation of new col lagen and elastin formation.9,14–16 In animal studies, after 10 minutes of exposure to temperatures of 39°C–43°C, the amount of collagen increased from an average of 9% before therapy to 25.9% after a 3-month follow-up period compared with no change in the untreated areas.4,17 Clinical studies on RF-assisted liposuction have shown up to 25% area contraction at 6 months and 35%–40% area contraction achieved at 1 year.10,18–20 Other studies have similarly shown through electron microscopy that collagen fibrils had a greater diameter after RF treatment. In addi tion, Northern blot analysis has confirmed microinflam mmatory stimulation of fibroblasts and other substances that enhance dermal structure.21 RF has not only been proved effective for skin tightening, but it has also been studied and proved effective in diminishing adipocytes.14 A number of RF applications are available to apply this energy in different ways (monopolar, bipolar, mul tipolar, and microneedling). The 2 RF delivery meth ods (bipolar RF and fractional bipolar RF) used in this study help achieve different treatment goals. The bipolar RF applicator uses a small 1.8-mm diameter, 13-cm long, silicone-coated RF-emitting probe. This directs electrical current flow from the internal to the external electrodes connected by the handpiece. As current is applied, the heat coagulates subcutaneous fat in close proximity to the internal probe and denatures the reticular dermis but pre serves the papillary dermis. The controlled heating allows for immediate tightening of the collagen triple helix via breakdown of hydrogen bonds in the collagen, causing shrinkage of the normal collagen structure, as well as induction of the healing cascade, leading to neocollagen esis, elastin remodeling, and angiogenesis over the follow ing 3–4 months.9 In addition, using a parachute analogy, the application of heat tightens the overlying fibroseptal networks (strings) and serves to uniformly contract the overlying skin (parachute). Complications are minimized by internal and external temperature, and impedance probes to rapidly detect (10×/ms) the soft tissue environ ment and automatically turns off RF energy if beyond the preset safety parameters (Figs. 1, 2).
In bipolar RF, the penetration depth is half of the dis tance between the electrodes, meaning the energy does not reach beyond the epidermis. Many attempt to circum vent this limitation by combining RF with other technolo gies to penetrate deeper, such as application of a vacuum to thin skin, infrared light pretreatment to change imped ance, or cooling procedures to increase the penetration depth.4 In this study, the effect of bipolar RF treatment was augmented by performing fractional bipolar RF in the same session. Fractional bipolar RF (Fractora modified to Morpheus8; InMode Aesthetics) deploys RF-emitting needles at variable programmable depths and energies depending on the region being treated. Unlike fractional CO2 or erbium, the fractional bipolar RF resurfacing can induce 3 types of effects—minimal superficial ablation for dyschromias and rhytids, controlled dermal coagula tion for tissue renewal, and overall volumetric heating for collagen stimulation.4 Fractional photothermolysis creates thermal injury that tapers as it descends deeper. In con trast, fractional bipolar RF creates zones of dermal injury narrowest at the epidermis with conical enlargement as the microneedles descend.10 When the RF needles penetrate deep into the dermis, there is a “molding” component of the subdermal adipose tissue which we term “subdermal adipose remodeling.” Hruza et al16 reported that 90% of patients with skin types II–IV showed an improvement in smoothness and rhytids, and 87% had improved in skin tightness. Seo et al13 compared facial soft tissue lax ity improvement with RF versus surgical facelift using blinded grading of photographs. They demonstrated a 49% improvement in skin laxity relative to baseline for the surgical facelift compared with 16% for the fractional
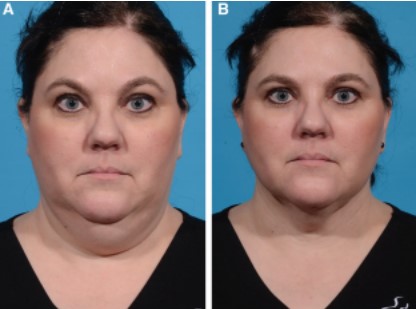
Fig. 1. Results of radiofrequency-assisted liposuction with fractional bipolar radiofre quency. A, The patient pretreatment. B, The patient 12 months postoperative.

Fig. 2. Results of radiofrequency-assisted lower face and neck treatment with fractional bipolar radiofrequency. A, the 64-year-old female patient pretreatment. B, results 24 months postoperative.
bipolar RF. Further, the mean laxity improvement from a single fractional bipolar RF treatment was 37% of the surgical facelift.13 Peterson et al22 also studied objective measurements of mechanical skin properties and demon strated a statistically significant improvement (5%–12% decrease in Young’s modulus and 10%–16% decrease in retraction time), as well as 1.42 grade improvement on the Fitzpatrick scale for wrinkles, and 0.66 on the Alexiades scale for skin laxity, increasing to 1.57 and 0.70 improve ment at 6 months. Patient satisfaction was noted to be “very high” for >90% of patients.22 A clinical study of the microneedle fractional bipolar RF handpiece (Intensif handpiece; EndyMed, Caesarea, Israel) demonstrated a significant improvement after 2 sessions and after 4 and 12 weeks of follow-up.6 A similar system (Scarlet, Korea) was studied in 3 consecutive sessions 4 weeks apart. Immunohistochemical staining (fibrillin-1) showed a sig nificant increase in dermal collagen content at 4 weeks after 3 sessions when compared with the baseline, as well as a significant increase in fibrillin-1 density from the dermal–epidermal junction to the deep dermis compared with the baseline.23
Other studies have demonstrated the efficacy of com bined multimodal RF application for facial aesthetic pur poses. Kaplan et al used 3 RF delivery methods together (nonablative skin tightening, RF fractional skin resur facing, and microneedling RF) on 14 subjects, showing improvements (>50%) in skin texture, laxity, and rhytids in 43% of the cohort without adverse effects or a signifi cant downtime.24 Previous studies have shown the efficacy of nonablative multisource RF as a single modality for face/body contouring.15,20,25 Other studies have shown the efficacy of RF microneedling as a single modality26 and the efficacy of a combination of nonablative RF and fractional skin resurfacing.27 Similarly to our findings, Mulholland in Hruza et al. identified the benefit of combining bipolar RF and fractional RF, stating that combining these applica tions allows for thermal stimulation for an “inside-outside dermal stimulation,” which can induce both an ablative rejuvenation of dyschromia, fine lines, and rhytides and a nonablative deeper dermal tightening.16 Our study find ings were consistent with Mulholland’s conclusion that combination therapy can deliver safe and consistent soft tissue rejuvenation.
The anatomic dissections performed as part of this study demonstrated the important surgical anatomy rel evant to this procedure. Specifically, the marginal man dibular nerve was found to be always above the inferior border of the mandible while anterior to the facial artery. The position was more variable posterior to the facial artery, in which case it was above the inferior border of the mandible in majority of cases. Importantly, consistent with prior anatomic studies, at approximately 2cm from the oral commissure, the marginal mandibular nerve divides and subdivides to enter the lip depressors. At this anatomic location, the skin and underlying muscle planes are closely adherent. It is for this anatomic reason that we elect to not treat areas medial to the marionette lines. Using this anatomic knowledge and aforementioned access ports, we found no nerve injuries (ie, transection, neuropraxia) and no extension of the device heat sig nature in proximity to the marginal mandibular nerve, consistent with the relatively low complication rate in the clinical arm of the study.
CONCLUSIONS
Combination therapy of bipolar RF and fractional RF had a positive effect on reducing the Baker Face/Neck Classification rating. When considering possible control variables, older patients were more likely to benefit from a larger magnitude of the treatment effect (as demonstrated by a decrease in the Baker rating from pre- to posttreat ment) compared to younger patients. However, both groups did demonstrate significant improvements across time.
Erez Dayan, MD
Avance Plastic Surgery Institute
5570 Longley Lane, Suite A
Reno, NV
E-mail: drdayan@avanceinstitute.com
PATIENT CONSENT
Patients provided written consent for the use of their images.
REFERENCES
- Alster TS, Graham PM. Microneedling: a review and practical guide. Dermatol Surg. 2018;44:397–404.
- Brightman L, Weiss E, Chapas AM, et al. Improvement in arm and post-partum abdominal and flank subcutaneous fat deposits and skin laxity using a bipolar radiofrequency, infrared, vacuum and mechanical massage device. Lasers Surg Med. 2009;41:791–798.
- Chia CT, Theodorou SJ, Hoyos AE, et al. Radiofrequency-assisted liposuction compared with aggressive superficial, subdermal liposuction of the arms: a bilateral quantitative comparison. Plast Reconstr Surg Glob Open. 2015;3:e459.
- Fritz K, Salavastru C. Ways of noninvasive facial skin tightening and fat reduction. Facial Plast Surg. 2016;32:276–282. 5. Iriarte C, Awosika O, Rengifo-Pardo M, et al. Review of appli cations of microneedling in dermatology. Clin Cosmet Investig Dermatol. 2017;10:289–298.
- Sadick NS, Makino Y. Selective electro-thermolysis in aesthetic medicine: a review. Lasers Surg Med. 2004;34:91–97.
- American Society of Plastic Surgeons. New statistics reveal the shape of plastic surgery; 2018. Available at https://www.plastic surgery.org/news/press-releases/new-statistics-reveal-the-shape of-plastic-surgery. Accessed November 10, 2018.
- American Society of Aesthetic Plastic Surgery. Cosmetic sur gery national data bank statistics. Aesthet Surg J. 2018;38(suppl 3):1–24.
- Hodgkinson DJ. Clinical applications of radiofrequency: nonsur gical skin tightening (thermage). Clin Plast Surg. 2009;36:261– 268, viii.
- Sadick N, Rothaus KO. Minimally invasive radiofrequency devices. Clin Plast Surg. 2016;43:567–575.
- Dayan E, Chia C, Burns AJ, et al. Adjustable depth fractional radiofrequency combined with bipolar radiofrequency: a mini mally invasive combination treatment for skin laxity. Aesthet Surg J. 2019;39(suppl 3):S112–S119.
- Irvine Duncan D. Nonexcisional tissue tightening: creating skin surface area reduction during abdominal liposuction by adding radiofrequency heating. Aesthet Surg J. 2013;33:1154–1166.
- Seo KY, Yoon MS, Kim DH, et al. Skin rejuvenation by micronee dle fractional radiofrequency treatment in Asian skin: clinical and histological analysis. Lasers Surg Med. 2012;44:631–636.
- Hantash BM, Ubeid AA, Chang H, et al. Bipolar fractional radio frequency treatment induces neoelastogenesis and neocollagen esis. Lasers Surg Med. 2009;41:1–9.
- Harth Y. Painless, safe, and efficacious noninvasive skin tighten ing, body contouring, and cellulite reduction using multisource 3DEEP radiofrequency. J Cosmet Dermatol. 2015;14:70–75.
- Hruza G, Taub AF, Collier SL, et al. Skin rejuvenation and wrin kle reduction using a fractional radiofrequency system. J Drugs Dermatol. 2009;8:259–265.
- Weiss R, Weiss M, Beasley K, et al. Operator independent focused high frequency ISM band for fat reduction: porcine model. Lasers Surg Med. 2013;45:235–239.
- Theodorou SJ, Paresi RJ, Chia CT. Radiofrequency-assisted lipo suction device for body contouring: 97 patients under local anes thesia. Aesthetic Plast Surg. 2012;36:767–779.
- Theodorou SJ, Del Vecchio D, Chia CT. Soft tissue contraction in body contouring with radiofrequency-assisted liposuction: a treatment gap solution. Aesthet Surg J. 2018;38(suppl 2):S74–S83.
- Royo de la Torre J, Moreno-Moraga J, Munoz E, et al. Multisource, phase-controlled radiofrequency for treatment of skin laxity: correlation between clinical and in-vivo confocal microscopy results and real-time thermal changes. J Clin Aesthet Dermatol. 2011;4:28–35.
- Zelickson BD, Kist D, Bernstein E, et al. Histological and ultra structural evaluation of the effects of a radiofrequency-based nonablative dermal remodeling device: a pilot study. Arch Dermatol. 2004;140:204–209.
- Peterson JD, Palm MD, Kiripolsky MG, et al. Evaluation of the effect of fractional laser with radiofrequency and fractionated radiofrequency on the improvement of acne scars. Dermatol Surg. 2011;37:1260–1267.
- Seo KY, Kim DH, Lee SE, et al. Skin rejuvenation by microneedle fractional radiofrequency and a human stem cell conditioned medium in Asian skin: a randomized controlled investigator blinded split-face study. J Cosmet Laser Ther. 2013;15:25–33.
- Kaplan H, Kaplan L. Combination of microneedle radiofre quency (RF), fractional RF skin resurfacing and multi-source non-ablative skin tightening for minimal-downtime, full-face skin rejuvenation. J Cosmet Laser Ther. 2016;18:438–441.
- Elman M, Vider I, Harth Y, et al. Non-invasive therapy of wrinkles and lax skin using a novel multisource phase-controlled radio frequency system. J Cosmet Laser Ther. 2010;12:81–86.
- Elawar A, Dahan S. Non-insulated fractional microneedle radiofrequency treatment with smooth motor insertion for reduction of depressed acne scars, pore size, and skin tex ture improvement: a preliminary study. J Clin Aesthet Dermatol. 2018;11:41–44.
- Elman M, Harth Y. Novel multi-source phase-controlled radio frequency technology for non-ablative and micro-ablative treatment of wrinkles, lax skin and acne scars. Laser Ther. 2011;20:139–144.